Before you can be sure you are struggling with the symptoms of sleep apnea, it is essential first to visit a credible sleep laboratory to allow the sleep specialist to diagnose sleep apnea before beginning to explore the treatment options available for treating sleep apnea syndrome.
Simply put, you cannot treat sleep apnea based on mere self-appraisal. You need a sleep specialist to diagnose you with sleep apnea and recommend the right therapy suitable for your conditions
What happens during the diagnosis process?
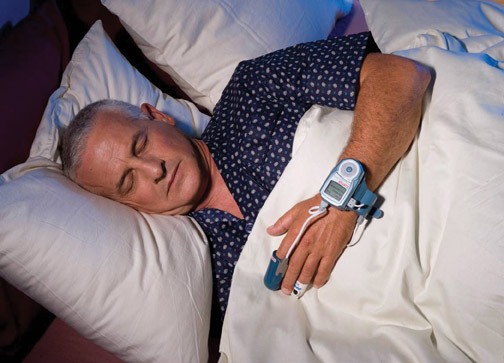
When you begin to notice the symptoms of mild sleep apnea, your doctor will make a holistic evaluation considering your sleep disorder symptoms and sleep history. After that, he may have to conduct a home sleep apnea test on his bed partner to have a balanced report.
Depending on the sternness of your sleep apnea symptoms, your sleep doctor may refer you to a sleep disorder center where a sleep specialist can help determine the nature of your symptoms and suggest the best treatment option.
A complete sleep study usually involves monitoring your breathing pattern and how other body parts function during sleep at the sleep laboratory. Home sleep apnea testing is a good option if you have the financial capacity to shoulder the bills. Some of the standard tests performed to diagnose sleep apnea include and is sleep apnea dangerous:
Nocturnal polysomnography
During this test, your doctor will hook you to equipment monitoring your lung, heart, and brain activities, including breathing patterns and arm and leg movements. He will also check your blood oxygen levels when you are sleeping.
Home sleep tests
Here, your doctor would prescribe some simplified tests you can run to diagnose sleep apnea at home. These tests measure your heart rate, airflow, blood oxygen levels, and breathing patterns. If he suspects central sleep apnea, your doctor may recommend polysomnography in a sleep testing facility rather than a home sleep test.
If the results do not detect symptoms of sleep disorders, your doctor might be able to prescribe a therapy without further testing. Portable monitoring devices might not sometimes detect sleep apnea. So your doctor’s provider might recommend polysomnography even if your previous results are within the standard range.
If you have obstructive sleep apnea, your healthcare provider might refer you to a specialist to remove the blockage in your nose or throat. In addition, you may also need an evaluation by a cardiologist or a neurologist to look for the causes of central sleep apnea.
What are the Treatment Options Available?
Continuous positive airway pressure (CPAP) therapy
If your test confirms you are struggling with mild sleep apnea, your doctor may only recommend changing a few things in your lifestyle, such as losing weight, quitting smoking, or exercising. You may also need to change your sleep position if necessary. If you have nasal allergies combined with obstructive sleep apnea, your doctor may recommend treatment for your allergies.
Your doctor may suggest several other treatments if the abovementioned measures don’t improve your symptoms.
Specific devices can help open a blocked airway. In other cases, surgery might be necessary.

Therapies for Obstructive Sleep Apnea
Continuous positive airway pressure (CPAP) machine
If you are diagnosed with moderate or severe obstructive sleep apnea, using a CPAP machine that supplies air pressure through a mask might benefit you. With Continuous Positive Airway Pressure (CPAP) therapy, the air pressure is greater than the surrounding air. However, it is enough to keep your upper airway passages open, preventing sleep apnea and loud snoring.
Other airway pressure devices
If using a Continuous Positive Airway Pressure machine continues to be a problem, you might use a different type of airway pressure machine that automatically adjusts the air pressure while sleeping. In addition, you can also access the units that supply bilevel-positive airway pressure (BPAP).
Oral appliances.
Wearing an oral appliance made to keep your throat open is another good option. Meanwhile, CPAP is more effective than oral appliances. However, oral appliances might be easier to use. Some or all devices are designed to keep your throat open by bringing your jaw to the front, which can relieve mild obstructive sleep apnea.
Several devices are available from your dentist. However, you might need to try different devices before finding one that works.
Surgery for Obstructive Sleep Apnea
Surgery may be a good option for people with Obstructive Sleep Apnea, but usually only after other treatments have failed. Generally, at least a three-month trial of different treatment options is suggested before considering surgery. However, surgery is an excellent first option for a small number of people with specific jaw structure problems.
Surgical options might include:
Tissue removal
During this procedure, a surgeon removes tissue from the rear of your mouth and the top of your throat. Your doctor might remove your tonsils and adenoids as well.
This surgery might successfully stop throat structures from vibrating and causing snoring. However, it is less effective than Continuous Positive Airway Pressure and isn’t considered a standard treatment for obstructive sleep apnea.
Jaw repositioning
In this surgery, the jaw is moved forward from the remainder of the facial bones. That enlarges the space behind the tongue and soft palate, making obstruction less likely. This procedure is among the quickest way to treat obstructive sleep apnea syndrome.
Implants
Your doctor may surgically implant soft rods made of polyester or plastic into the soft palate after numbing you with a local anesthetic.
Nerve stimulation
It requires surgery to insert a stimulator for the nerve that controls tongue movement. The increased stimulation helps keep your tongue in a position that keeps your airway open.
Creating a new airway
You may need this surgery if other treatments have failed or you have severe sleep apnea. In this procedure, your surgeon opens your neck and inserts a plastic or metal tube through which you breathe.
Therapies for Central Sleep Apnea
Treatment for medical problems
Causes of central sleep apnea may include neuromuscular disorders, and treating those conditions might help. Other therapies that may be used for Central Sleep Apnea include supplemental oxygen, Continuous Positive Airway Pressure (CPAP), Bilevel Positive Airway Pressure (BiPAP), and adaptive servo-ventilation (ASV).

Medicine changes
You may be prescribed medications such as acetazolamide to help manage your breathing. However, if drugs worsen your Central Sleep Apnea, such as opioids, your healthcare provider may change your medications.
Supplemental oxygen
Using supplemental oxygen when sleeping might help if you struggle with severe central sleep apnea. Your doctor will also help you choose the correct form of oxygen available with devices to supply oxygen to your lungs.
Adaptive servo-ventilation (ASV)
The new airflow device observes your typical breathing pattern and stores the information in a computer. Then, after you fall asleep, the machine uses pressure to control your breathing pattern and prevent pauses.
Final Words
is it advisable that you first seek the help of your sleep specialist before taking any step to treat symptoms of sleep apnea? Meanwhile, you must be sure you approach a specialist treating sleep apnea issues to get the best result.
Also Read:
- Sydney Sleep Study Cost Compared: Clinic vs At-Home Testing
- Bulk-Bill Sleep Study Sydney: Where to Find No-Gap Options
- ResMed AirFit F40 vs. Fisher & Paykel Evora: Which Minimalist Full Face Mask Wins?
- Home Sleep Study Brisbane: Is It as Accurate as In-Clinic Testing?
- Home Sleep Study Adelaide: How It Works and Who It’s For
